BVCHD has been recognized with two important patient safety honors: BETA HEART Award for validation in 5 domains and the Emergency Department (ED) Quest for Zero Tier 2 Award.
This year marks the organization’s 7th consecutive year of participation in the BETA HEART program.
BETA HEART is an extensive program that includes five domains that pertain to responding to harm events and encouraging transparency with the patient and family. BETA HEART is based on a philosophy of Healing, Empathy, Accountability, Resolution and Trust. There are five domains to the program that include: Culture of Safety, Rapid Event Detection, Investigation and Determination, Communication and Transparency, Care for the Caregiver and Early Resolution.
The Emergency Department’s Quest for Zero Harm Tier 2 Award further highlights its commitment to advancing safe, reliable, and high-quality care for every patient.
These awards reflect the dedication of physicians, nurses, and staff to building a strong culture of safety and reducing preventable harm. They also recognize the organization’s ongoing commitment to continuous improvement and patient-centered care.

At Bear Valley Community Healthcare District (BVCHD), patient safety and staff well-being are at the heart of everything we do. We are proud to foster a strong Culture of Safety — one that encourages open communication, shared accountability, and continuous improvement.
In 2018, BVCHD implemented a Just Culture program. The goal of Just Culture is to create a work environment where staff feel safe to speak up about concerns — whether it’s a near miss, a system issue, or a workaround that could put patients or staff at risk. Instead of focusing on blame, we focus on learning. By understanding what went wrong and identifying system improvements, we can prevent future harm and strengthen safe, reliable care.
As part of our ongoing safety efforts, BVCHD also promotes the Speak Up Campaign, which empowers staff, patients, and families to raise questions or concerns without hesitation. We believe that every voice matters when it comes to safety and quality.
Through these efforts, BVCHD is building a culture where transparency, respect, and collaboration ensure the best possible outcomes for our patients and our community.
At Bear Valley Community Healthcare District (BVCHD), we believe that every patient interaction is an opportunity to provide excellent care and a positive experience. Listening to our patients and families is one of the most important ways we learn and grow.
To capture feedback, we use NRC Experience surveys after Emergency Department visits, inpatient stays, and clinic visits. These surveys give us real-time insight into how patients feel about their care, helping us celebrate what we’re doing well and identify areas for improvement.
We also participate in the national Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey. HCAHPS sets a standard for measuring patient experience across hospitals nationwide. By taking part, BVCHD can compare our results locally, regionally, and nationally — and most importantly, use the feedback to make meaningful improvements in customer service, communication, and quality of care.
Your voice truly matters. The feedback we receive through these surveys helps guide our efforts to create a welcoming, compassionate, and patient-centered environment for every person who walks through our doors.
BVCHD has been proud to host an active Patient and Family Advisory Council (PFAC) since January 2017. The PFAC meets quarterly to provide feedback and guidance on patient- and family-centered care, including policies, admission information, and barriers to accessing or understanding healthcare at our facility.
The council is made up of community members who volunteer their time to improve care at BVCHD. Each member has either been a patient or is a family member of a patient, bringing a unique perspective that helps us see care through the eyes of those we serve. Over the years, their ideas and contributions have led to meaningful improvements and strengthened our connection to the community.
PFAC members also play a role in celebrating our staff by participating in the DAISY Award (for extraordinary nursing) and the STEM Award (for excellence in support, technical, and essential medical roles). These programs recognize employees who go above and beyond, reinforcing a culture of appreciation and compassion.
Patient and Family Advisors are selected through an application and interview process and serve as volunteers for a one-year term, with the option to re-apply for a second year. BVCHD is continually recruiting new advisors who have been a patient or family member of a patient within the past two years and who are willing to collaborate with leadership in a positive and constructive way.
We are always looking for passionate community members to serve on the Patient and Family Advisory Council (PFAC). If you or a loved one have received care at BVCHD within the past two years, we welcome your perspective to help us improve the patient experience. PFAC members volunteer their time, meet quarterly, and collaborate with hospital leadership to bring positive change.
To learn more or apply, please contact Tracy Lewis 909-878-8261.
At Bear Valley Community Healthcare District (BVCHD), we believe data is a powerful tool for improving patient safety, quality, and experience. Through our partnerships with the Hospital Quality Institute (HQI) and SpeedTrack, we are able to collect, analyze, and act on key information that drives better outcomes for our patients and our community.
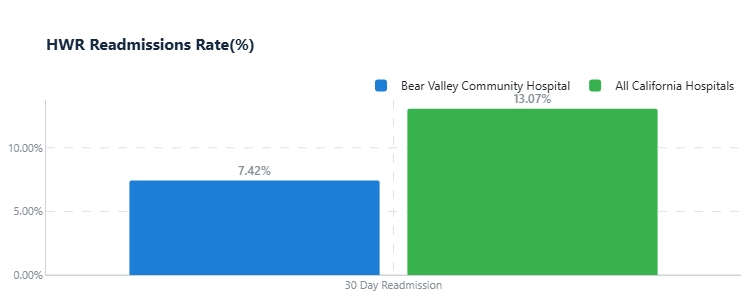
We regularly review data on hospital readmissions, social determinants of health (SDOH), and diagnosis-specific trends to identify gaps in care and opportunities for improvement. This allows our teams to focus on issues most relevant to our patients — such as medication management, follow-up care, and access to resources.
Transparency is a cornerstone of this work. By sharing our readmission data and other measures publicly, we hold ourselves accountable and demonstrate our commitment to continuous improvement. More importantly, we use these insights to design initiatives that directly impact the patient experience — from improving discharge education, to expanding community health programs, to addressing barriers like housing and transportation.
At BVCHD, data isn’t just numbers on a chart — it’s a way to listen, learn, and take action to ensure safe, reliable, and compassionate care for every patient.
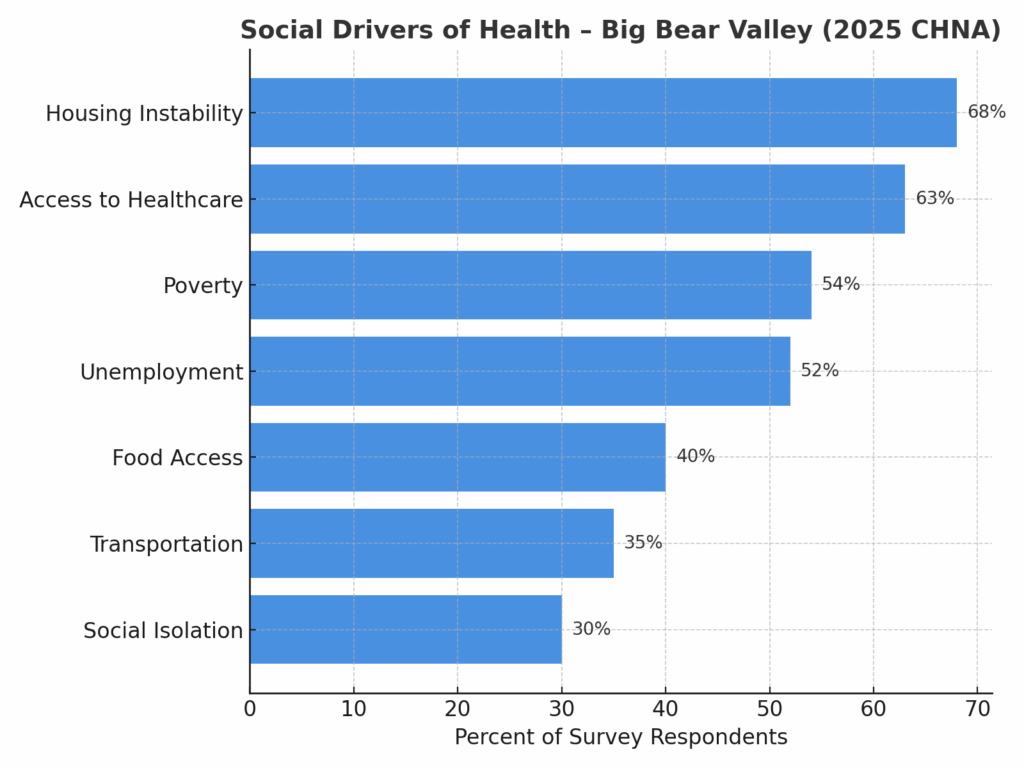
At Bear Valley Community Healthcare District (BVCHD), we know that health is shaped by much more than medical care. Where people live, work, learn, and play—often called social drivers of health (SDOH)—have a direct impact on overall well-being.
Through our 2025 Community Health Needs Assessment (CHNA), we learned that community members are most concerned about:
We share this information publicly because improving health requires strong partnerships across our community. By listening to residents and tracking SDOH data, BVCHD can work with local organizations, schools, businesses, and policymakers to address these challenges and create a healthier Big Bear Valley for everyone.
Bear Valley Community Healthcare District partners with Health Services Advisory Group (HSAG), which is contracted with CMS as the Quality Improvement Organization (QIO) for California. HSAG provides support and guidance to both hospitals and Skilled Nursing Facilities (SNFs), helping strengthen quality and safety across the entire continuum of care.
Priority areas include care coordination, patient safety, behavioral health, and prevention of chronic disease. HSAG also supports providers with emerging quality topics such as supply chain management, medication shortages, disaster preparedness, and workforce planning.
For SNFs, HSAG places special emphasis on reducing hospital readmissions, enhancing infection prevention and control, and improving resident care coordination and engagement. Through education, data sharing, and best-practice resources, HSAG helps ensure patients and residents receive safe, high-quality, and coordinated care — whether in the hospital or post-acute setting.
Bear Valley Community Healthcare District (BVCHD) is proud to be recognized as a Stroke Ready rural hospital, ensuring our community has access to timely, lifesaving stroke care close to home. Our dedicated team follows the latest evidence-based practices to provide rapid diagnosis, treatment, and stabilization, giving patients the best possible outcomes.
In recognition of this commitment, BVCHD has been honored with the American Heart Association’s Get With The Guidelines® Gold Award for 2024—the highest level of rural recognition in the AHA GWTG Stroke program. This achievement reflects our team’s dedication to delivering fast, high-quality stroke care right here in our mountain community.
The Centers for Medicare & Medicaid Services (CMS) created the Hospital Star Rating system to help patients and families compare the quality of care across hospitals. The ratings are based on multiple measures, including safety, outcomes, patient experience, and readmissions.
As a Critical Access Hospital (CAH), Bear Valley Community Healthcare District provides essential care to our rural community. Because of our smaller size and lower patient volumes, we often do not have enough cases reported for CMS to generate a star rating. This does not mean that quality data isn’t collected — it simply means there are not enough patients in certain categories for CMS to produce a score that can be compared fairly to larger hospitals.
At BVCHD, we are committed to transparency and continuous improvement. While a star rating may not be available for our hospital, we regularly track and share quality data, patient experience feedback, and safety outcomes through our partnerships with organizations such as HQI, SpeedTrack, and HSAG. This ensures that our community can trust the care we provide, even when national reporting systems cannot reflect it.
The BVCHD Skilled Nursing Facility is committed to deliver the highest quality of care to residents and takes a proactive approach to improving services through the Quality Assurance/ Performance Improvement program. The QAPI program is ongoing, comprehensive and deals with a full range of services offered by the facility. The scope of the program encompasses all systems of care and management practices including but not limited to resident/family feedback, staff satisfaction, individualized resident care plans, clinical care and resident safety.
SNF QAPI workgroups meet regularly to review performance data, identify areas in need of improvement, and carry out and monitor improvement efforts. For these activities, teams will use a variety of QI approaches and tools, including Performance Improvement Plans (PIPs), Plan Do Study Act (PDSA) cycles, workflow mapping, assessments, audit and feedback, benchmarking, and best practices research.
The SNF is certified by the Centers for Medicare and Medicaid Services. CMS regularly publishes data showing comparisons of nursing homes through data gathered from facility surveys, staffing reviews, and quality of care indicators.